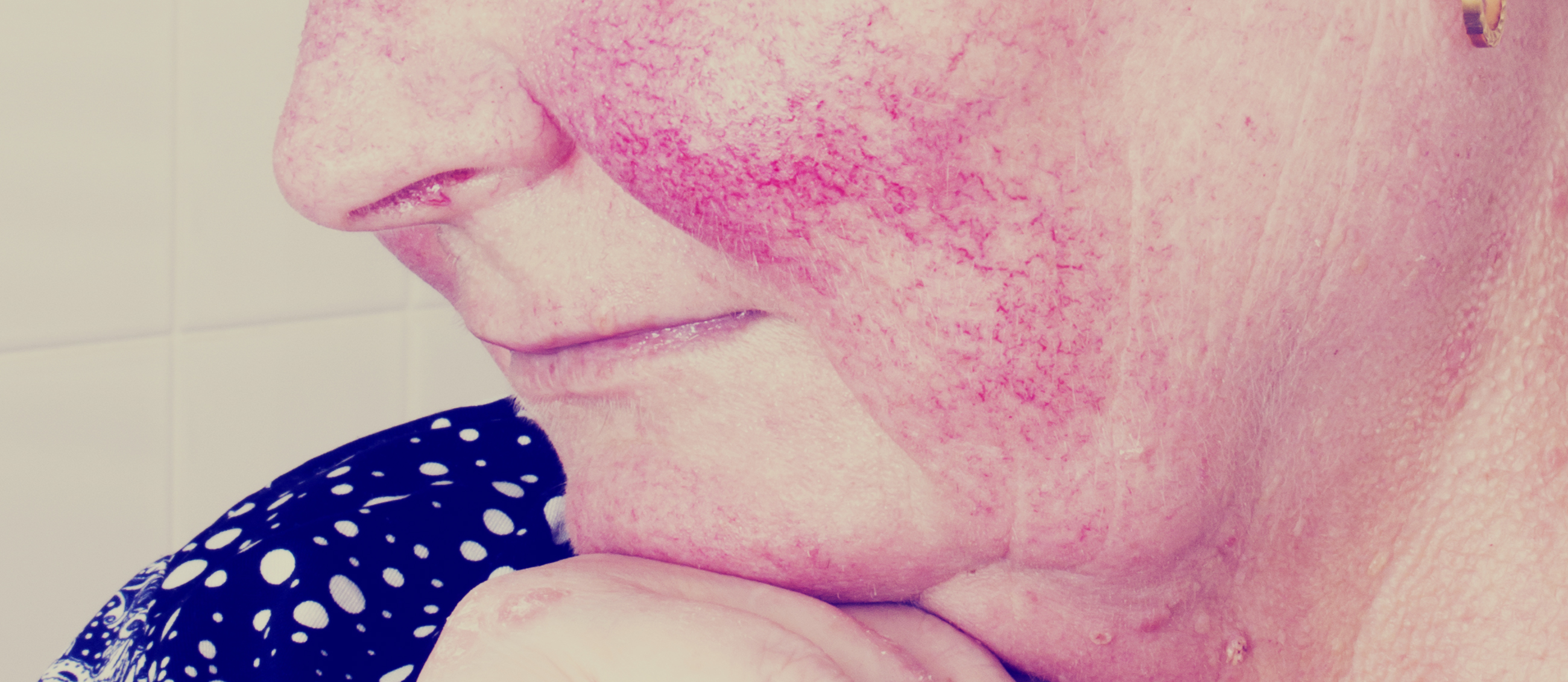
What is rosacea?
Rosacea, or acne rosacea, is chronic skin disorder affecting the curves and features of the middle of the face. It is characterised by one or more of the following primary features: flushing (erythema), which can be transient or non-transient; papules and pustules; telangiectasia (the symptom of threadlike red lines or patterns that may cross the face of rosacea patients).[1]
It can also result in rhinophyma, whereby the tissue on the nose thickens and has a bulbous appearance.[2] Women aged from 30 years and of a Caucasian background appear to have a greater risk of rosacea.[3]
Due to the visible nature of rosacea, sufferers can experience low self-esteem, embarrassment and frustration. To assist with quality of life, symptom suppression is a primary treatment goal.[3]
The main allopathic treatments are aimed at inhibiting inflammatory pathways via topical medications such as metrondidazole and oral low dose antibiotics, with the only approved oral drug for rosacea listed as doxycycline.[3]
What are the causes of rosacea?
Currently, the pathogenesis of rosacea is unknown,[3] but it seems it has a multifactorial aetiology with both genetic and environmental factors playing a role.
In some individuals, mites on the surface of the skin called Demodex follicular trigger up-regulation of toll-like receptor 2 (TLR2) in skin cells. This immune response causes inflammation of the skin[4] and points to an innate immune disruption in rosacea.[5]
Other microbial exposures that have been associated with rosacea include: Bacillus oleronius, Staphylococcus epidermidis, Helicobacter pylori and Chlamydophila pneumoniae.[4]
Both genetic and epidemiological studies have shown pathogenic links between rosacea and gastrointestinal disorders, including H. pylori.[6] One single-arm study that tested this hypothesis found that when H. pylori was eradicated the signs of rosacea were reduced.[7]
Further evidence that rosacea may be influenced by dysbiosis is, when compared to controls, people who had rosacea had an increased prevalence of gastrointestinal disorders such as small intestinal bacterial overgrowth (SIBO), Crohn’s, ulcerative colitis, irritable bowel syndrome (IBS) and coeliac disease.[6]
Several studies have shown clustering of autoimmune conditions including type 1 diabetes, rheumatoid arthritis, multiple sclerosis and coeliac disease in some people. It is hypothesised that rosacea also meets this criteria, with an association between autoimmune conditions and rosacea most noticeable in females.[2]
Interestingly, three human leucocyte antigen (HLA) alleles and two single-nucleotide polymorphisms (SNPs) have been identified to be associated with rosacea.[3] Hopefully the identification of these gene variants may shed some light on the mechanistic link between gene variants and rosacea type and treatment, with further research warranted.[3]
What are the treatment options for a natural medicine practitioner?
The role of the diet in rosacea
Dietary modifications have become an accepted part of rosacea treatment,[8] as some food and drinks may aggravate rosacea. Generally these foods fall into the following categories: heat, alcohol, capsaicin and cinnamaldehyde-related. The possible mechanism may be due to neurogenic vasodilation via the “activation of transient receptor potential cation channels”.[5]
A simple way of managing a rosacea flare is to avoid or limit spicy foods, alcoholic beverages and hot or caffeinated drinks. But each individual needs to find their “triggers” which may also include fruits, marinated meats and cheese.[8] Dietary changes are a modifiable lifestyle factor a practitioner can easily use alongside other interventions to assist in reducing symptoms and flares of rosacea.[5]
Treat dysbiosis
Some authors suggest the reason why antibiotic therapy may assist in the treatment of rosacea is because it is addressing the underlying infection or dysbiosis,[5] therefore potential treatment options could include prebiotics and probiotics.
One particular probiotic that has demonstrated benefit is Saccharomyces boulardii (SB). SB has been shown to interfere with cellular signalling pathways common in many inflammatory conditions. It also improves eradication rates of H. pylori when used alongside triple therapy, as well as being effective in reducing flareups of ulcerative colitis and IBS[9] - all conditions linked with rosacea.
Probiotic therapy in general help reduce dysbiosis. It has been demonstrated that dysbiosis of intestinal bacteria results in “activation of plasma kallikrein-kinin pathways”[5] which then goes on to trigger neurogenic inflammation. Probiotics also provide protection via a number of mechanisms including: a general anti-inflammatory action via alleviation of T-cell mediated skin inflammation, reduction in reactive oxygen species (ROS) and improvement of skin barrier function.[5]
To rule out dysbiosis, practitioners could recommend their patients undertake non-invasive testing for signs of infection/dysbiosis including SIBO or H. pylori breath tests.
Treat immune disruption and potential autoimmune component
There are a number of naturopathic methods to treat immune dysregulation and autoimmunity. The key nutrients that show the most evidence to treat rosacea are:
Vitamin D
A higher prevalence of vitamin D deficiency in patients who have rosacea and other autoimmune diseases has been noted.[2] Vitamin D plays a role in protecting the mucous membranes of the intestines as well as acting as a mediator of epithelial defences.[10] Therefore addressing the potential inflammation and dysbiosis component of rosacea. Direct sunlight can irritate rosacea[5] so it is best to keep the face covered and instead expose the limbs directly to sun, as well as considering vitamin D supplementation.
Zinc
Studies in to the usage of zinc as a treatment for rosacea have been limited. (Weiss), However, zinc is a fundamental nutrient in cell mediated immunity and as an anti-inflammatory.[5] Zinc also plays a role in maintaining the epithelial barrier function in both the gastrointestinal system and the skin,[11] so any gut healing protocol is worthy of its inclusion.
Reduce inflammation
The innate immune disruption seen in rosacea leads to a pro-inflammatory cascade, thus the use of anti-inflammatory agents would be useful as part of a treatment protocol.[5] Omega-3 acts as an anti-inflammatory by competitively inhibiting pro-inflammatory pathways,[5] and turmeric could also be an adjunct to current rosacea therapy due to its ability to modulate inflammation.[12]
Further research is needed as to the gut-skin connection in rosacea. However, with the emergence of antibiotic resistance,[5] an opportunity exists for natural therapists to work alongside allopathic medicine to reduce severity of rosacea symptoms and potentially address the underlying causes of this condition, which can be tied up in autoimmunity, gut health and dietary allergens.
References:
- Staedtler G, Shakery K, Endrikat J, et al. An empirically generated responder definition for rosacea treatment. Clin Cosmet Investig Dermatol 2017;10:347-352. [Full Text]
- Egeberg A, Gislason GH, Hansen PR, et al. Clustering of autoimmune diseases in patients with rosacea. J Am Acad Dermatol 2016;74(4):667-672. [Abstract]
- Rainer B, Kang S, Chien AL. Rosacea: Epidemiology, pathogenesis, and treatment, Dermato-Endocrinology 2017;9(1):e1361574. [Full Text]
- Weinkle A, Vladyslava D, Emer J. Update on the management of rosacea. Clin Cosmet Investig Dermatol 2015;8:159-177. [Full Text]
- Weiss E, Katta, R. Diet and rosacea: the role of dietary change in the management of rosacea. Dermatol Pract Concept 2017;7(4):31-37. [Full Text]
- Egeberg A, Weinstock LB, Thyssen EP, et al. Rosacea and gastrointestinal disorders: a population-based cohort study. Br J Dermatol 2017;176(1):100-106. [Abstract]
- Saleh P, Naghavi-Behzad M, Herizchi H, et al. Effects of Helicobacter pylori treatment on rosacea: A single-arm clinical trial study. J Dermatol 2017;44(9):1033-1037. [Abstract]
- Keri J, Rosenblatt AE. Literature review. J Clin Aesthet Dermatol 2008;1(3):22-26. [Full Text]
- Kelesidis T, Pothoulakis C. Efficacy and safety of the probiotic Saccharomyces boulardii for the prevention and therapy of gastrointestinal disorders. Therap Adv Gastroenterol 2012;5(2):111-125. [Full Text]
- Assa A, Vong L, Pinnell LJ, et al. Vitamin D deficiency promotes epithelial barrier dysfunction and intestinal inflammation. J Infect Dis 2014;210(8):1296-1305. [Abstract]
- Skrovanek S, DiGuilio K, Bailey R, et al. Zinc and gastrointestinal disease. World J Gastrointest Pathophysiol 2014;5(4):496-513. [Full Text]
- Gupta SC, Patchva S, Aggarvwal BB. Therapeutic roles of curcumin: lessons learned from clinical trials. AAPS J 2013;15(1):195–218. [Full Text]
DISCLAIMER:
The information provided on FX Medicine is for educational and informational purposes only. The information provided on this site is not, nor is it intended to be, a substitute for professional advice or care. Please seek the advice of a qualified health care professional in the event something you have read here raises questions or concerns regarding your health.