If you haven't heard of Lara Briden, you're not listening. Lara is a force in integrative medicine who has written books, chapters of texts, podcasted, blogged and treated thousands of happy patients, both male and female, who selected her for her expertise in treating hormonally-related issues.
In today's podcast, Lara covers the many drivers of polycystic ovarian syndrome (PCOS). Lara delves into just what hormones become dysregulated and what we, as natural healthcare practitioners, can do about it.
Lara Briden will be speaking at the 2020 BioCeuticals Symposium, if you would like to hear her speak in person, register your ticket today.
Covered in this episode:
[00:30] Welcoming back Lara Briden
[01:36] What is PCOS, and what isn't it?
[05:08] Assessment methodology
[12:08] Is PCOS over-diagnosed?
[13:33] Genetics: what role is this playing?
[15:09] Other drivers of PCOS
[21:48] Endocrine Disrupting Chemicals (EDCs)
[23:14] Post-pill PCOS
[26:11] Dietary and Lifestyle Interventions
[32:55] Herbs and Nutrient interventions
[35:02] The ATMS PCOS Symposium 2018
With thanks to:
Andrew: This is FX Medicine, I'm Andrew Whitfield-Cook.
Joining us on the line today from New Zealand is Lara Briden, who's a Sydney naturopath with more than 20 years' experience. She first trained as a naturopathic doctor in Canada and then moved back to Sydney in 2001.
Lara is a passionate communicator about women's health and alternatives to hormonal birth control. Her book, the "Period Repair Manual," published by Pan Macmillan and now in its second edition, is a manifesto of natural treatment for better hormones and better periods, and provides practical solutions using nutrition, supplements, and natural hormones. The book has been an underground sensation and has worked quietly to change the lives of tens of thousands of women. And Lara will also be speaking at the ATMS Symposium in Sydney on the 16th of September 2018. We'll be speaking about the drivers of PCOS, and that's what we're here to today to discuss.
Welcome back to FX Medicine, Lara. How are you?
Lara: Hi. Well, Andrew. Thank you so much for having me.
Andrew: Now, I was enamored by the first time you joined us in on FX Medicine and indeed when I heard you speak at the 2017 ATMS Symposium. That was just an awesome, awesome educational experience.
But today, we're going to be talking about something that...there is a lot of circulatory sort of things happening here with PCOS. So I think we first have to get a definition. What is PCOS and what isn't it?
Lara: That's a very good place to start. Because the condition is, I'll venture to say, rather loosely defined. Unlike some other women's health problems, such as endometriosis, which is a very specific disease, PCOS is best defined as kind of a group of symptoms. In that way, it's an umbrella diagnosis because I think women can come to that place for a lot of different reasons physiologically.
But most fundamentally, the group of symptoms are irregular periods, so irregular ovulation, and then the second key symptom is excess male hormones. And so there are different, as I have discovered in my work and through the research there is, there are different drivers or processes that can bring a woman to that place of having those two main symptoms.
Andrew: And like my historical background of this, when it was...I think people started to first define it and they tried to over-define it. There was apple shaped obesity, there was the hirsutism, there was the cardiovascular paradigm in there as well. But that's not always present, as I now understand it. Is that correct or not?
Lara: That's correct, because it's really, I'll say, it's kind of an assortment of a few different conditions. I think that qualifies for the diagnosis of PCOS. Which is why I really think we need a new name for the condition, that's in the works potentially. To define it based on androgen excess. And I would propose we perhaps even need a few different names, depending on to what degree there are insulin resistance or some of the cardiovascular parts of the picture. In my view, that's kind of a distinct condition.
Andrew: And, like, I also remember the PCOD, polycystic ovarian disease. So there was this attempt to define it as a disease rather than a syndrome, as you say, collection of symptoms. And the other part of it is there is also polycystic ovaries.
Lara: Which is not a thing.
Andrew: Which is not a thing.
Lara: I'll say, for what it's worth, that ultrasound finding of polycystic ovaries, on its own, without any other evidence of problem, is not a condition, it doesn't define anything. And it's actually really...I'm glad this came up near the beginning of our conversation because there has been a trend to over-diagnose PCOS based on that ultrasound finding.
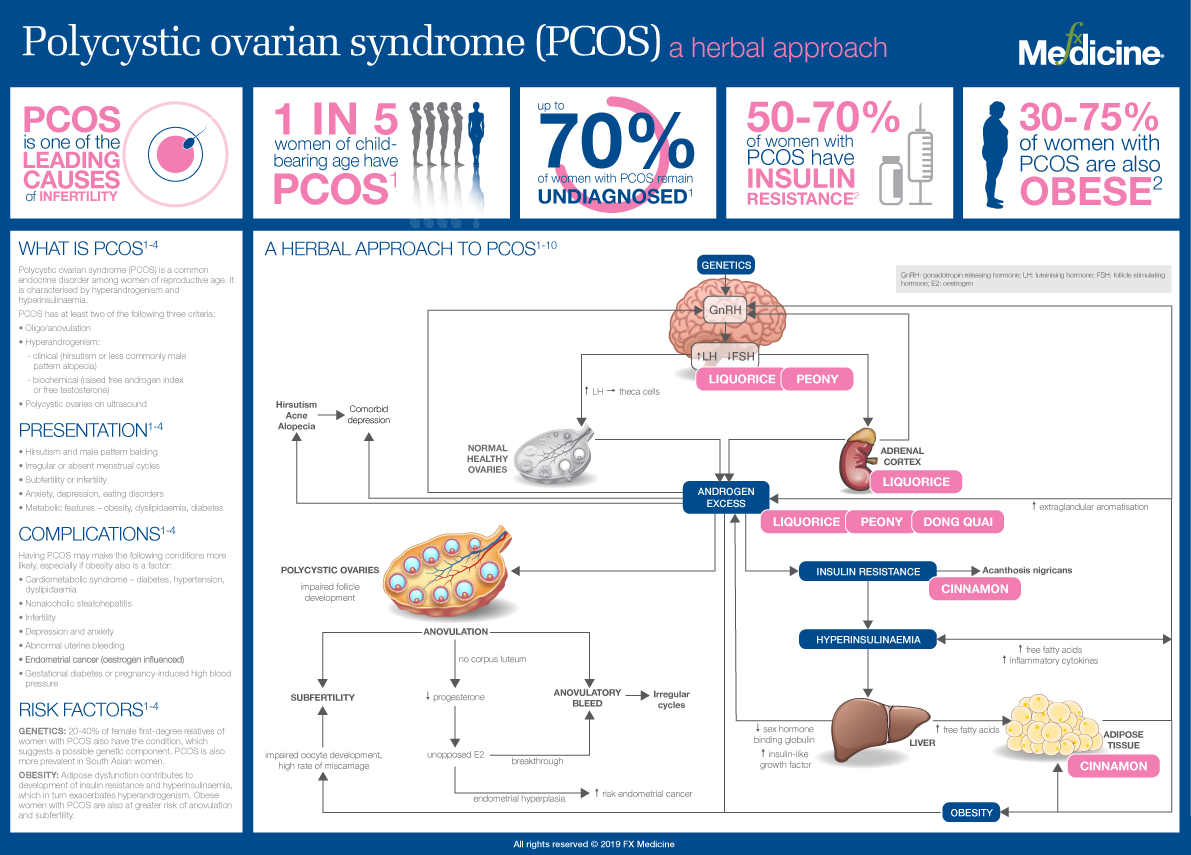
Polycystic Ovarian Syndrome (PCOS) A Herbal Approach - INFOGRAPHIC
So you might have women who just came off the pill, for example, or have lost their periods because they're undereating, or there’s lots of different scenarios. And many of those women will show up with polycystic ovaries on ultrasound, but they don't have the androgens and the insulin resistance and some of the other things going on.
So their doctor says to them they have PCOS and then they're looking essentially in all the wrong places for the solution of what they need to do. And that's a lot of what I do in my clinic, is working through that confusion and trying to guide women to a more accurate assessment.
Andrew: Okay, so what do you do to arrive at that? Do you look at levels of androgens? Do you look at perhaps some cardiovascular markers or indeed doing a fasting insulin? Do you look at that sort of thing?
Lara: I do do a fasting insulin. I'll give you my little flowchart. So step one is the big question of do you have, do you qualify for PCOS diagnosis? Which would mean, is there some evidence of an ovulation or ovulatory dysfunction and is there some evidence of excess male hormones?
So that evidence for the male hormones could be male hormones on blood tests. Not saliva tests, I'll say at this point. You cannot pick them up as saliva test. So if you do see elevated male hormones on saliva test it's not accurate, I will venture to say. Or may not be accurate. And then blood test is what I use.
So I will test testosterone, DHEAS, androstenedione, some of the androgens, and also at the same time look for elevated prolactin and rule out some other conditions. You can use the blood test to rule out other conditions that can cause elevated androgens.
So that's step one. Also, the blood test for evidence and the second evidence for androgens would be clear physical symptoms like facial hair, body hair, a particular pattern of hair loss, perhaps acne although acne on its own not a defining symptom of androgen excess. And if that's all present and then I can say, "Yes you definitely do seem to be qualifying for a PCOS diagnosis at least at this stage," then the next step in the flowchart is...and you said it just a couple of minutes ago, is do you have insulin resistance? That's the very next question to answer.
Andrew: One of the other big surprises for me as well was how I immediately pigeonholed women into this, particularly the body shape, the apple-shaped obesity, that sort of thing. And yet I've met quite a few women now who have PCOS and are the fittest, some, in some cases, slimmest, trimmest women that I know. And yet they have this issue that they constantly battle against.
Lara: Absolutely. Yes.
Andrew: How do we break that picture? How do you.... When somebody is presenting with you, what's the key thing that you go, "Hang on, there is something happening here."
Lara: Well, again, it, you know, if they qualify for that first step of the irregular ovulation and the high androgens, then we know there is something going on.
So then the next step is to determine if they have insulin resistance. That usually means that testing either fasting insulin or a glucose tolerance test with insulin, it's not enough to just test the blood glucose or even, I would argue, even just a normal glucose tolerance test, and then determine if insulin resistance is present.
So just as you said, it may be present...even a lean woman, a not overweight woman can have insulin resistance. So that's why that testing is so important, you just can't assume it's like, "Oh, you're skinny therefore this is not what's happening." So that step is very important.
But then there are… because of the nature of the way this condition is loosely diagnosed or defined, there are then going to be some women who are qualifying for PCOS but don't have that main underlying driver of insulin resistance.
Andrew: Oh okay.
Lara: So then it becomes a bit more of put on the detective hat and try to identify what has, for that particular woman, what has kind of, pushed her into the state of high androgens. Recognising that for anyone who moves into a state of high androgens there is going to be some underlying genetic tendency to do so.
Andrew: Right, got you.
Lara: It's sort of a mismatch with the environment. They...for whatever reason, have a combination of genes that they have under certain pressures whether it be, you know, insulin resistance or other pressures coming off the pill might be an example. They then move into this hormonal state, and it's reversible. This is the other thing that's important to understand, I mean, we hear that, you know, there is no cure for PCOS. I would say that's true in that women who have this tendency, probably a genetic tendency, are always going to battle against it to some degree.
But the consensus amongst the experts that I have spoken to, and myself included in this camp, I think for many women the symptoms are reversible therefore by definition once you don't have active symptoms you really move out from under that diagnosis, yeah.
Andrew: You don't have the syndrome.
Lara: You might move in and out of it, like you might have it and then it's like, "Oh, no, you're clear." And then you move back in.
But the other thing that happens with PCOS is you tend to outgrow it. So there was recently a paper, Australian paper called...I'm trying to get the exact name. It came out in the British Medical Journal just a few months ago, saying...they called it Are Expanding Diagnostic Criteria Causing Over Diagnosis Amongst Women for PCOS was basically the title.
And they make a few points, one that I said earlier, that ultrasound on its own is not adequate for diagnosis. And they also make the point that many women, this is something more of a problem when they're young, so most teenagers are in kind of a mild state of PCOS anyway, that's kind of normal for them. And then, you know, as you move into your 20s, 30s, a lot of that will, for many women, will tend to improve on its own. So that's something important. In that paper, they're saying that's important to communicate that women so that they don't get too scared. Because it's quite frightening to be told that there is something wrong with your ovaries, but in reality for many of them, it's possibly just a stage that they're in.
Andrew: And indeed, I guess once anybody, any woman in this case, gets a diagnosis, it can be either or both an answer, a relief to know what's going on. But also once you know that there’s something, let's use the word ‘wrong’, that they can then go through even like a grieving period, a shock period to adjust to.
Lara: Absolutely. Well, I guess how I would describe it is they can kind of freak out, you know, be very scared, and start taking a lot of treatments including diet that they might not need. And even just the anxiety around that can worsen the condition.
So I'm trying to reframe the condition a little bit. I know it can be very serious for some women but for many women who have been given that label of PCOS, it's relatively probably quite a mild situation and doesn't mean they're not going to be able to have babies or anything like that long-term.
Andrew: The interesting thing is when I was nursing, this didn't exist. It just never came up.
Lara: Yeah.
Andrew: And then it was basically as soon as I finished nursing, and then this term started to be bandied round and became more and more and more common. So is it a case that we're picking it up and answering questions that we overlooked before, or is it really becoming more common?
Lara: It's both. It's being over-diagnosed. At least in Australia, I'm convinced of that. And that's explained in the British Medical Journal paper that I mentioned.
But at the same time, I think there is a growing trend to the problem and I think one of the main reasons that's becoming more common in the last few decades is because of insulin resistance. So as we know, metabolic syndrome or insulin resistance is becoming more common. There a couple of key reasons for that, probably. But one of the downstream effects of that for women is PCOS.
Andrew: Okay, so in the meantime, I just found that reference, it's Tessa Copp, the reference is "Are expand diseases definition unnecessarily labeling women with polycystic ovarian syndrome?" It's BMJ 2017 for everybody. We'll put that up on the FX Medicine website for you to review. That's brilliant, Lara.
I just wanted to go on, you mentioned genetics before, and I have to ask the question, is part of this that obesity, calorie-conserving gene that we unfortunately have favoured through the ice age in human development, human evolution, and now, of course, we've got overabundance of calories so it's now our downfall. Is that one of the issues? And what other triggers do you see with PCOS?
Lara: So with regards to metabolic syndrome type of PCOS, yes, that's pretty close to the situation, I think. That some of us in the population have ancestors who were well adapted to famine. You can see that as a superpower, really. You know, they were able to keep making babies, reproducing even in the face of low food supply, which was great for them. But now there is a mismatch with our modern world, not just in terms of excess food supply generally but in terms of sugar specifically.
I think when a diet high in fructose hits that genome, kind of combines with that thrifty metabolism, as they call it, the results can be insulin resistance. And that we know from the research that that's actually compounding each generation that's exposed to this diet, which is, I think, one of the reasons that we're just seeing such a rapid growth in the incidence of insulin resistance which is quite worrying and not just for PCOS, but for all the other downstream effects of that.
Andrew: And what about other drivers like, for instance, the ‘big baddie’ of all conditions is inflammation. Or runaway inflammation, self-propagating inflammation, rather than resolving-inflammation. What’s the issue here and is it driven by hormones, or are hormones driven by it?
Lara: Again, with PCOS specifically… I put it through the lens of… what… for this individual patient, what is the thing that is interfering with her ovulation? Her regular ovulation. And what is the thing that is skewing her to high androgens instead of, a progesterone, for example. And for about 70% of women who qualify for the PCOS diagnosis, the thing that’s pushing them there is insulin resistance.
Then there’s about 30% of women for whom, there’s no evidence of insulin resistance. There seems to be something else going on. And amongst that group, yes, there is a smaller group of women for whom the chronic inflammation is perhaps one of the biggest driving factors. I actually refer to that in my book and in my work as ‘inflammatory PCOS’.
It’s not to say that there’s no inflammation involved in the other types. Because of course, there’s kind of a metabolic inflammation that comes from insulin resistance itself.
Andrew: Yeah, it’s a driver, yeah.
Lara: So that’s part of the dysfunction. That’s part of the picture. But I guess when I say ‘inflammatory PCOS’, I’m talking about the smaller sub-group of women who maybe have more of the kind of, immune inflammation related to food sensitivities and gut microbiome problems and that kind of chronic inflammation. And that does seem to be a trigger or a driver for some women. But, again, I’ll say, it’s not the majority. In general I don’t think of PCOS as an inflammatory condition the way I would say, endometriosis, in contrast.
Andrew: Right.
Lara: But, so yes, you’re right. I think it certainly plays a role, for some women. And so, I’ll just talk through the other two types of what I see, of what I call the ‘types of PCOS’.
So there’s the insulin resistance type, which is by far, the majority. And then, the inflammatory type I work with. And then, this post-pill PCOS as well, which we can talk about, if you like. And then finally, the fourth one is quite a small group of women, that are called, or I call that ‘adrenal PCOS’.
So these are women for whom, there’s actually quite a different situation going on. They got, their androgens, or male hormones are primarily from their adrenal glands and their ovaries do not seem to be affected as much. So that’s a different picture. And they, women like this, need different strategies than the classic PCOS.
Andrew: We often term this ‘adrenal fatigue’ and things like that, which I probably think is a misnomer because it’s the brain that changes in volume. But there’s a cross-talk. It’s the hormones that talk between these two organs and glands if you like. Are we talking about a stress-induced adrenal secretion of these hormones or is there some other mechanism there?
Lara: No, it’s pretty much… well, it’s stress-induced. Certainly stress can worsen it, once it’s established. Once there’s that patterns of excess male hormone from the adrenal glands, then one of the strategies is to reduce stress. To manage diet as well as using some of the natural medicines that help to regulate that brain-adrenal-HPA axis communication.
But what’s interesting about the adrenal PCOS, is that a little bit of research that I found has correlated it with stress during puberty. So particular… like whether a parent died or there’s something, like a bit hit of stress around that kind of, 13-14 year old age. Which, when I read that I thought that really makse sense. That matches with some of what I’m seeing with my patients. And it just kind of makes sense to me as a, you know, as a biologist and a clinician, that when the reproductive hormonal system is calibrating itself and maturing and becoming established. It’s learning, essentially, it’s environment. To have a big disruption like that at such an early age seems to have, well… I hate to say permanent, but kind of long-term effects.
Andrew: Yeah.
Lara: And, there can also… to be fair with the adrenal-type of PCOS, there can be… there’s clearly a role of environmental toxins as well. Like hormone disrupting chemicals, as well. There’s going to be a genetic component to that, as there is with any condition, really.
So, it’s worth mentioning. Because even though it’s only a small group of women, I’m sure there’s some of your listeners who have patients that fit into that category and might now be able to think “Yeah, ok, that gives me a different direction to take.”
Andrew: That's a really important point you make and I'm just...like, my mind is going down rabbit holes here, I'm wondering about EBV, you know, you've got hormonal priming?
Lara: Yep.
Andrew: You've got the perfect storm of stress hormones and infection as a priming sort of, let's say, an imprinting agent. And that's only a small section of PCOS.
Lara: Yeah, that would just be...yeah.
Andrew: Oh, that's the other thing….
Lara: Should we talk also...no, go ahead.
Andrew: I think it's really interesting as well, during periods of growth and development, bursts of growth and development like infancy and like puberty. The microbiota changes, the microbiome changes to favour the proteobacteria and then comes back in to sort of swing for other bacteria later on. It's really interesting what's happening here and I wonder, who knows? But I wonder if there is any sort of potential. Is there a potential place in which we can intervene here to re-balance things so that maybe they're not so permanent? I mean, that's a big question mark.
Lara: Yeah, you mean intervening with the microbiome, potentially.
Yeah, potentially, I mean, we know that changes with the microbiome can influence the HPA axis. And you're right about the influential windows. So you know when we're a foetus or when we're an infant or when we're in puberty, those are all very influential times, like little windows where we're more vulnerable, for example, to endocrine disrupting chemicals. We're probably more vulnerable, potentially, to microbiome-disrupting agents during those times, so unfortunately, some of us just, you know, get unlucky if you get the wrong kind of stress during that vulnerable time.
Andrew: So let's talk about these EDCs, because this is something that's...I mean, they're ubiquitous in our environment. We're now...we're not talking about plastics now, now we're talking about microplastics.
Lara: Endocrine-disrupting chemicals is a broad group so it includes obviously plastics, pesticides would probably be a pretty big one in that group, heavy metals as well. Especially lead and mercury are endocrine disrupters. And, you know, they have the flame retardants in furniture and also fire retardants in...yeah, there is lots of different factors. That's almost a whole podcast on its own. And obviously, I'm not fully up to speed on all the different nuances of that or even how much...I'm not even sure how much we even know at this stage. Because I find it's quite a burden for patients to have to think about that and try to avoid things. I give them common-sense advice to avoid any unnecessary pesticides, but at the same time, I don't want them to become anxious about it because I think...in reality for most of us, I think especially for something like PCOS, I think some of the damage was done when they were exposed as a teenager or exposed in-utero or whenever it was. So, I mean, all we can do is, for their condition, is use the tools that we have, which are, you know, diets and supplements and herbal medicine. And also as a society, I think work to reduce the burden of toxins that are affecting the next generation.
Andrew: This is obviously a smaller segment of the women that are affected with PCOS, Lara. What about some of the other types? Obviously, you're going to be delving into this at the ATMS Symposium later on in this year, but can we discuss maybe the post-pill type of polycystic ovarian syndrome?
Lara: Yes, let's do that. So after the insulin-resistant type, which is the most common, I would say the post-pill type is the next most common.
Post-pill PCOS is not an official designation, unfortunately. I mean, that's what I call it, that's what a number of my fellow clinicians call it. It's a very real thing that we see in clinic. There's almost no research into it, which is kind of disturbing.
So it's a situation where someone was fine before they went on the pill, maybe they were on the pill for 10 or 15 years, and come off and then get a surge in androgens, you know, can't get their ovulations going, probably have some post-pill acne show up, polycystic ovaries on ultrasounds, and panic, basically.
And I think a few things I'll share about that for the listeners is, number one, that can be a temporary state. I'm really confident to say that.
Andrew: Right.
Lara: But that is...sometimes it's a longer-term state, but sometimes they just need 12 months or so to recover from the steroid drugs of the pill, essentially, and to start to ovulate and for their ovaries to get their groove back and stop making so much testosterone.
The endocrinologist who helped with my book, Professor Jerilynn Prior, she described that kind of situation, maybe sort of post-pill PCOS. As temporary...what did she call it? Temporary, adaptive, anovulatory androgen excess. So she's kind of saying this is just a moment in time where… the reason of coming off the pill, the ovaries sort of move into this temporary state of not really doing what they're supposed to. And it's understandable given how strong those drugs are and the suppression the ovarian function has been under for the 10 or 15 years on the pill. It's not a surprise that it can take them a while to recover.
And what makes me sad is when women are given that diagnosis they just, of course, accept it as that they have disease, they have a long-term condition, they're going to need metformin, they're going to need IVF or whatever is it. It just kind of quickly snowballs out of control. Because often they'll have come off the pill to fall pregnant and then they just feel like they're on this really short time frame, they really don't want to wait 12 months for their periods to come back and their androgens to come back to normal. So they start more interventions straight away, and that makes me quite sad, obviously.
Andrew: And there’s the stress driver.
Lara: Yes, and then the stress is making it worse, yes. So I guess my advice would be to come off the pill sooner rather than later.
Andrew: Right, okay. Let's talk a little bit about interventions, and obviously, this is going to be a huge area. But from what you're saying about the insulin resistant-type being the most common, are we really saying, okay, how do we intervene? Diet and lifestyle. Is it just diet and lifestyle, diet and lifestyle, diet and lifestyle?
Lara: Diet is huge for that first type, that insulin resistant type. Which is the majority of women who qualify for the PCOS diagnosis. They need to quit sugar, that's how I see it. You know, I'm in the camp that feels that the high dose fructose is one of the biggest inducers of insulin resistance. So I'm quite clear with my messaging around this because I see a lot of women… patients kind of struggling, quite confused about a low carb diet and trying to cut potatoes and every other thing and feeling hungry all the time and yet still having you know, paleo desserts and smoothies and fruit juice.
So I just want to be clear that for insulin resistance the most effective dietary intervention, I feel, I find, is to remove those dessert-type foods. So sweetened yogurt, fruit juice, dates.
Andrew: Do you have to quit sugar totally or can you still have a teaspoon?
Lara: No, there is a sweet spot, actually, this is in my book.
So there’s...fructose is interesting. Because there is a… up to about 25 grams of fructose, which is not grams of total carbohydrates, that's just specifically fructose. Up to about 25 per day is actually quite healthy and improves insulin sensitivity. So that would equate to about three pieces of fruit in the day, for example.
Anything above that, depending on your genetic situation and your sensitivity, can start to induce insulin resistance. And it's not that hard to have more than 25, as you can imagine. Like, if you're having fruit juice and sugar in your coffee and date balls and smoothies and sweetened yogurts, you can be up in the 100, 150 grams of fructose per day. Which, is obviously quite different than the 25.
So yeah, when I speak about fructose I speak specifically more about the quantity, and my little rule of thumb if it's dessert then it's too much fructose… if it's essentially dessert it's too much fructose. But if it's whole fruit, that's different.
Andrew: What about the message, though, about saying, okay, they're having their three pieces of fruit so they're "healthy," but they're also having three cups of coffee a day with one, or, heaven forbid, two, I used to. Then they're driving things way up.
Lara: Yeah, no, the sugar in the coffee has to go. So if my patients, if that's very stressful for them to think about not having that sweetener, then I might look at temporarily using stevia or xylitol or something like that to give them that sweet sensation and help them come off.
Andrew: What about lifestyle interventions, Lara? Historically this has been the big brick wall to success of therapy. How do you start it, particularly when they already might have a weight issue, and how do you keep them on the golden path?
Lara: So we're talking about exercise, which is very effective, very important it improves insulin sensitivity. With my own patients I almost never speak about weight loss anymore, I speak about insulin sensitivity, I speak about the metabolic benefits of exercise for their own sake. Not as a way to lose weight.
Because I feel like perhaps, what I've observed with some of my patients is, when they get discouraged is when they're doing everything right and they're not seeing the scale change, for example, that just seems to throw them right off.
So I will say, "Look, I don't know exactly what's going to happen with your weight, I'm confident that in the long term your body is going to find a new set point, it's going to come to the weight that's healthy for it. But in the shorter term, we're just focused on health. And we're specifically focused on getting your insulin down.. well, into a normal range.” Not down too low. But certainly, with fasting insulin, I like to see it below eight, between about four and eight. That's for any clinicians listening out there. And that gives a metric that you can track with patients, which I think they find quite helpful.
So you can say, "Okay we're going to stop sugar, concentrated sugar, we're going to do some exercise, you know, eat full solid meals, get sleep, and then we're going to recheck your insulin in a few months and that's going to give you that positive feedback that you're doing things right."
Andrew: What about different types of exercise? You know, HIIT therapy, I guess with regards to dietary measures, and you've also got things like intermittent fasting. But with lifestyle interventions, with exercise, do you ever employ specific types of exercises or techniques?
Lara: I’d like to more, because I've also seen that research about the value of strength training and it's pretty convincing.
So in terms of counseling my own patients, I do mention strength training. I don't have the knowledge to kind of direct them specifically. So even as we're talking, I'm thinking I need to give them a bit more direction with that. Because strength training doesn't have to be complicated. You know, I started doing, just on my own, kind of squats and pushups and...what's great about strength training is some of it you can just do at home.
Andrew: What about keeping people on that? What about long term success with therapy? Do you ever find that people...that the best method of keeping people on track is to have these regular visits? That the gaps between visits lengthens but that regular visitation, just to make sure that they're still cool with what's happening, checking in biochemically as well, I guess. Make sure everything is on the right track with regards to their hormones and their insulin resistance and things. Do you ever find this sort of long-term guidance is the best way to go?
Lara: Yeah, well, the great thing about being a woman, I'll say, is we have this handy barometer of our health, which is our period. So with my patients, patients with PCOS, it's like if you can stay at the point where your period is coming regularly and your androgen symptoms are improving, then that's your feedback that you know you're doing the right thing. And when you start having sugar again and stop doing exercise, the periods are going to become irregular again, you're going to start to get some of the other symptoms of PCOS.
So it's quite a handy feedback mechanism in that way. But every individual is going to be different. Certainly, I've had patients who are, I guess, not at the right points in their life to take that in, or maybe I'm just not the right person to be telling them. But not everybody can just quit sugar and run with it, no, it's obviously...they have to have their own individual, personal reasons why they want to do that.
Andrew: Yeah. Let's look at other therapies like herbs and nutrients. In the past, there's been these old favorites like gymnema and bitter melon and things like that. Do you find any...I am a full advocate of individualising therapy so I'm not saying we should be prescriptive about this. But do you ever find there is sort of go-to herbs and nutrients that you usually employ?
Lara: So there are a few that I mention in my book, of course, and I'm going to just, kind of state them now.
So we're talking now, for the, I guess, I'll say the classics type; the insulin-resistant type of PCOS. I'd say the number one is magnesium. It sensitises the body to insulin. I find it works...well, I'll say, I find/observe that it works as well as metformin with my patients and then it obviously has other benefits, too.
Andrew: Yeah.
Lara: So it's quite a nice treatment. Next down from that, some of the.. couple of nutrients that you need for ovarian signaling are zinc and vitamin D. Those are both quite important especially if they're deficient.
The next nutrient that gets a lot of research is something called inositol, myo-inositol, which helps with insulin signaling. It's done smashingly well in clinical trials for PCOS. Like, it's just, yeah, it's kind of the superstar for PCOS right now.
And the next one I'll mention, because there was recently some Australian research about it by naturopath Susan Arentz, on the herbal combination peony and licorice, peony and licorice. So that's available in tablet form by a couple of brands in Australia and I use that quite a lot. It helps to re-establish normal ovarian signaling and can also have an anti-androgen effect.
Andrew: Yeah, it's kind of this sort of hero TCM combination, wasn't it?
Lara: Yeah.
Andrew: It was almost two herbs that were just the..
Lara: Synergistic…
Andrew: …The stars.
Lara: Yeah, yeah.
Andrew: It almost became a term where two herbs joined for one name. It's ‘paeonylicorice’.
Lara: Exactly. So I use that quite a lot, and I also say, you know, I get good results. It's not just me, other clinicians and doctors are getting good results with that kind of protocol.
Andrew: As we've said before, you'll be speaking at the 2018 ATMS symposium in Sydney. What can delegates expect to learn from you, and indeed some of the other speakers? I know that you don't… aren’t up with all of their talks. But what's the general feel of things? What can we expect to learn from this symposium?
Lara: I think the main takeaway will be to look beyond just the label of PCOS. For example, my talk is called "Deep Diagnosis: The Different Drivers of PCOS and How To Treat Them." So it's kind of similar to what I talked about just now but in more detail, and I'll be citing more treatment ideas for each type.
And it's all part of an evolving understanding of PCOS but it's not just a polycystic ovary on ultrasound, it's a whole body hormonal condition and it's more than one. It's not just the one thing, it has different causes for different women. So it's important to look at the individual patient sitting in front of you and run through some of the questions that I mentioned, including; question number one, does she really have PCOS?
Andrew: I've got to say I really admire the way that you look further than a label. But I think one of the reasons that I most admire you for, Lara, is that you're not just dedicated to your patients but you're dedicated to your profession and spreading the word about better care for these women who are undergoing these issues, especially PCOS, which we discussed today. Thanks so much for joining us on FX Medicine.
Lara: Yeah, oh, thanks for having me.
Andrew: This is FX Medicine, I'm Andrew Whitfield-Cook.

Additional Resources
| Lara Briden |
| ATMS Special Event: PCOS Symposium, Sept. 2018 |
| Professor Jerilynne Prior |
Research explored in this episode:
Other podcasts with Lara include:
- Hallmarks of Healthy Menstruation
- Navigating Polycystic Ovarian Syndrome with Lara Briden
- FX Medicine LIVE at the 2017 ATMS Endometriosis Symposium
DISCLAIMER:
The information provided on FX Medicine is for educational and informational purposes only. The information provided on this site is not, nor is it intended to be, a substitute for professional advice or care. Please seek the advice of a qualified health care professional in the event something you have read here raises questions or concerns regarding your health.