Researchers from as far back as 1930 suspected a link between gut and skin health and this has certainly been a cornerstone of understanding for wholistic medicine practitioners. However, modern research is now confirming the importance of this relationship. Recent studies have indicated that small intestine bacterial overgrowth (SIBO) is 10 times more prevalent in those suffering acne rosacea compared to healthy controls. Also, patients suffering from inflammatory bowel disease (IBD) have a significant increase in skin manifestations.
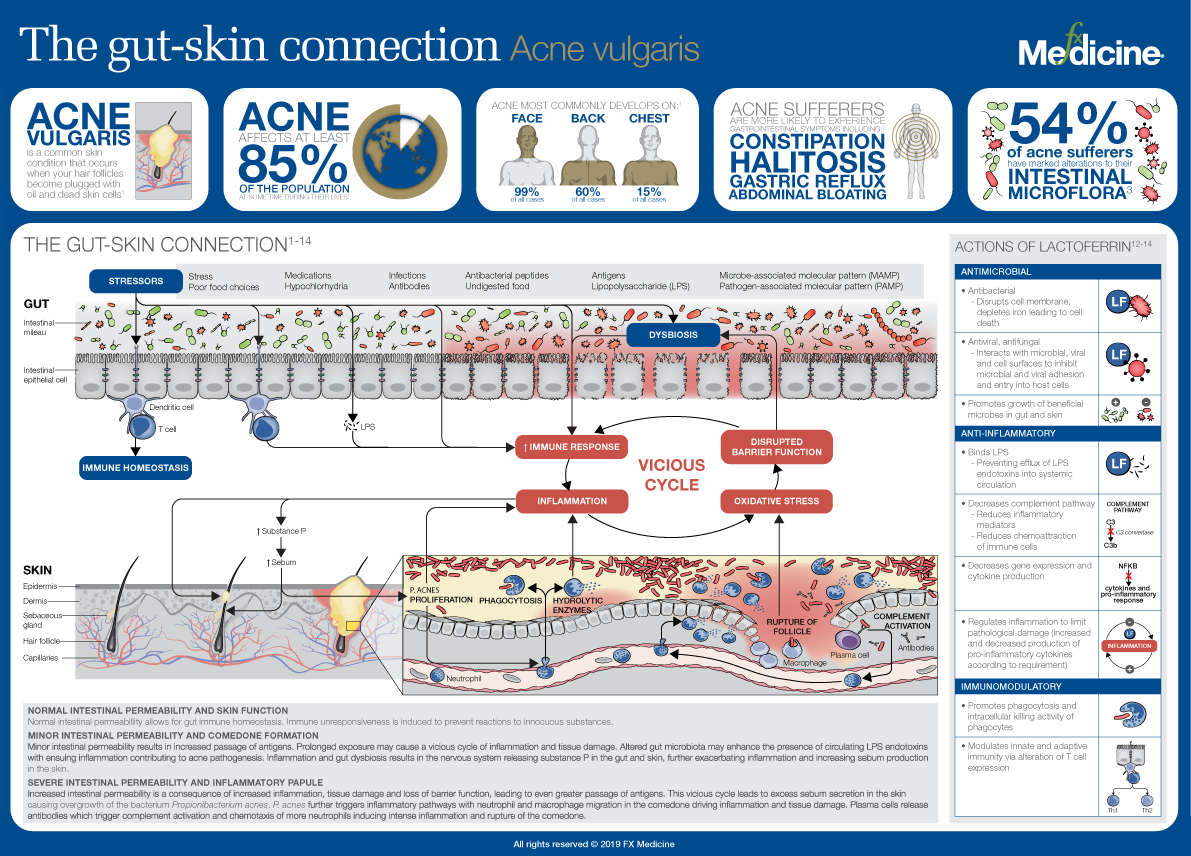
In this infographic, we explore the gut-skin connection. In particular, we look at the role of the gastrointestinal (GI) tract and its influence on acne severity via a systemic effect on inflammation, oxidative stress, tissue lipid levels, pathogenic bacteria, as well as levels of neuropeptides. Although acne is not being suggested as a condition purely of the digestive tract, there appears to be more than enough supportive evidence to suggest that gut microbes, and the integrity of the gastrointestinal tract itself, are contributing factors in the acne process. Through this understanding, the benefits of lactoferrin as an immune-modulating, anti-inflammatory nutrient, becomes a topic of practical interest and we review the mechanisms of action for its use in addressing acne.
References
- MyVMC. Acne. Virtual Medical Centre 2016. [Link]
- Bowe WP, Patel NB, Logan AC. Acne vulgaris, probiotics and the gut-brain-skin axis: from anecdote to translational medicine. Beneficial Microbes 2014;5(2):185-199. [Full text]
- Volkova LA, Khalif IL, Kabanova IN. Impact of impaired intestinal microflora on the course of acne vulgaris. Klin Med (Mosk) 2001;7939–7941. [Abstract]
- Rubin E, Farber JL. Pathology, 3rd Edition. Philadelphia: Lippincott Williams & Wilkins, 1999.
- Tan JK, Bhate K. A global perspective on the epidemiology of acne. Br J Dermatol 2015;172(Suppl 1):3-12. [Abstract]
- Ganceviciene R, Graziene V, Bohm M, et al. Increased in situ expression of melanocotin-1 receptor in sebaceous glands of lesional skin of patients with acne vulgaris. Except Dermatol 2007;16(7):547-552. [Abstract]
- Selway JL, Kurcab T, Kealey T, et al. Toll-like receptor 2 activation and comedogenesis: implications for the pathogenesis of acne. BMC Dermatol 2013;13:10. [Full text]
- Arck P, Handjiski B, Hagen E, et al. Is there a ‘gut-brain-skin axis’? Exp Dermatol 2010;19:401-405. [Full text]
- Grice E, Segre JA. The skin microbiome. Nat Rev Microbiol 2011;9(4):244-253. [Full text]
- Bowe WP, Logan AC. Acne vulgaris, probiotics and the gut-brain-skin axis - back to the future? Gut Pathog 2011;3(1):1. [Full text]
- Kober MM, Bowe W. The effect of probiotics on immune regulation, acne, and photoaging. Int J Women’s Dermatol 2015;85-89. [Full text]
- Gagnon L. Acne pathogenesis. Greater understanding yields new therapeutic targets. Dermatology Times. [Link]
- Kanwar JR, Roy K, Patel Y, et al. Multifunctional iron bound lactoferrin and nanomedicinal approaches to enhance its bioactive functions. Molecules 2015;20(6):9703-9731. [Full text]
- van der Walden WJFM, Blijlevens NMA, Donnelly JP. The potential role of lactoferrin and derivatives in the management of infectious and inflammatory complications of hematology patients receiving a hematopoietic stem cell transplantation. Transpl Infect Dis 2008;10(2):80-89. [Full text]
This image by FX Medicine is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
More information about how to share/use the infographics for personal use.
If you interested in using any FX Medicine content for commercial use please contact us.
DISCLAIMER:
The information provided on FX Medicine is for educational and informational purposes only. The information provided on this site is not, nor is it intended to be, a substitute for professional advice or care. Please seek the advice of a qualified health care professional in the event something you have read here raises questions or concerns regarding your health.



