According to recent statistics, the incidence of lactose intolerance in Australia has increased significantly. In the time period from 2011-2015 rates have risen from 2.8% to 4%. While this may not seem significant, an increase of 1.2% equates to an additional 240,000 people who are actively living with lactose intolerance. Interestingly, the overwhelming weight of this burden is being carried by women with 6.2% of Australian women suffering from lactose intolerance versus 1.7% of Australian men.[1]
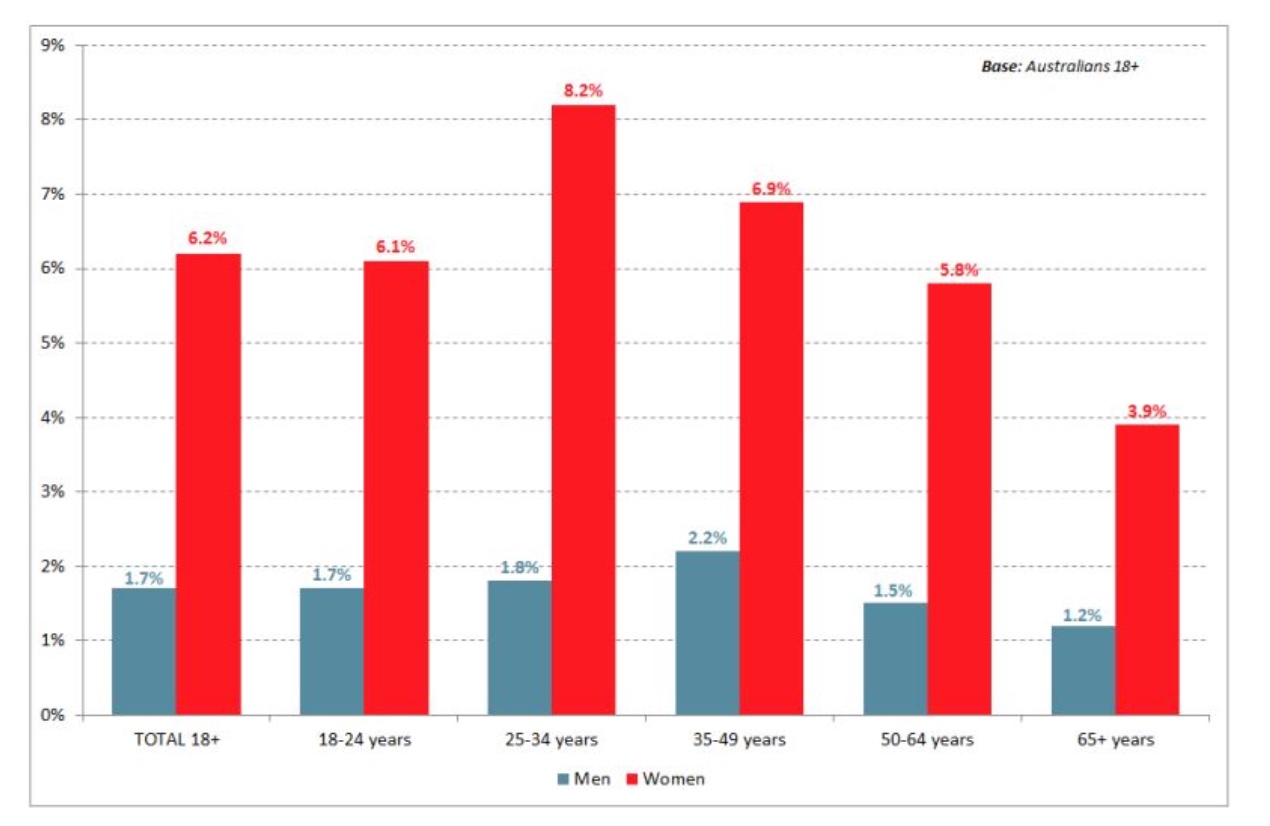
Picture: Prevalence of Lactose Intolerance in Men vs Women. [Source]
WHAT IS LACTOSE?
Lactose is a unique carbohydrate which is present exclusively in mammalian milk [1,2] and is the primary fuel for infant feeding. It is a disaccharide that is comprised of glucose and galactose.[4] Human milk contains approximately 7.2g/100mL of lactose, whilst cow’s milk contains 4.7g/100mL.[5] The carbohydrate content of human milk is essential to meet the energy demands of a baby’s rapid growth and development.[2] In order to yield the lactose for absorption and utilisation by the body, the intestinal brush border enzymes need to split the bonds linking the two monosaccharides.[3] This enzyme, lactase, is found throughout the small intestine and is particularly localised to the tips of the villi.[3]
Most mammals lose the ability to produce lactase after weaning resulting in deficient hydrolysis of lactose into its constituent monosaccharides. Undigested lactose is then metabolised in the large intestine by colonic bacteria, where anaerobic metabolism produces hydrogen and variety of metabolites.[4]
UNDERSTANDING LACTOSE INTOLERANCE
Lactose intolerance is typically referenced when side effects of milk consumption are experienced. Symptoms of lactose intolerance include abdominal pain, bloating, flatulence and diarrhoea.[2] However clinicians need to discern whether the side effects are as a result of the carbohydrate (lactose) or protein (casein) portion of the milk product(s) as this can affect what food products a person may then go on to consume.
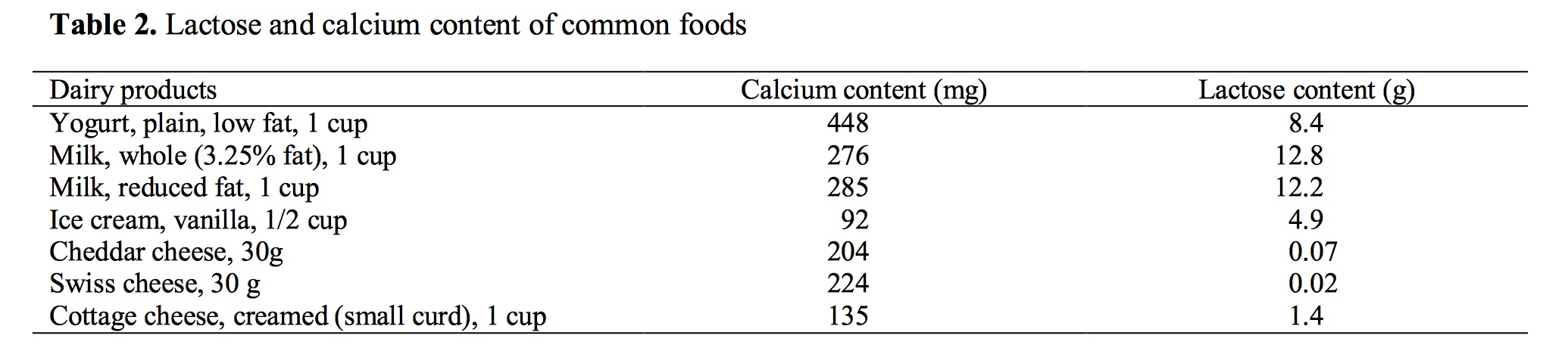
Not all dairy foods contain the same levels of lactose. See Table [6]
Cow milk–protein intolerance is reported in 2-5% of infants within the first 3 months of life and is typically resolved by 1 year of age.[3] Lactose intolerance is a distinct entity from cow milk–protein sensitivity, which involves the immune system and causes varying degrees of injury to the intestinal mucosal surface.[3] Congenital lactose intolerance is a very rare condition. However, lactase activity may be low and need to mature during the first weeks of life in many infants.[5]
Lactose intolerance has become embedded in Western medicine based on evidence that intestinal lactase activity persists into late childhood and throughout life in only a minority of the world’s population, notably northern European–derived populations. Genetically, these populations have a single nucleotide polymorphism (SNP) which positively influences the lactase LCT gene. Other lactase persistent (LP) populations are found in Africa and the Middle East with different genetic variants. These SNPs represent co-evolution with the advent of dairying culture since the agricultural revolution some 10,000 years ago and is considered a key driver to lactase persistence beyond weaning.[6]
PREVALENCE
In populations with a predominance of consuming dairy foods as few as 2% of the population has primary lactase deficiency. In contrast, the prevalence of primary lactase deficiency is 50-80% in Hispanic populations, 60-80% in black and Ashkenazi Jewish populations, and almost 100% in Asian and American Indian populations.[3]
The inability to digest milk after infancy has been labelled as a defect, when in fact it is the natural state of more than two-thirds of the world’s population. Young children can almost universally produce lactase and can digest the lactose in their mother’s milk. But as they mature, lactase gene expression is typically switched off as children are weaned. Only about 35% of the human population can continue to effectively digest lactose beyond the age of about seven or eight.[6]
Clinically, lactase deficiency can also occur following small bowel injury or assault, such as viral and parasitic infections. There is even some debate over whether there is a clinical necessity to keep lactose intake to a minimum following severe gastroenteritis (e.g. 1-3 weeks) due to the potential for intestinal damage.[5]
PATHOGENESIS
A lactose intolerant individual can tolerate up to 12-25g of lactose on any single occasion irrespective of lactase status.[6] However, this tolerance can be impacted by other factors such as food and meal pattern context, the health of the gut microbiota and age.[6] Some malabsorbers have been shown to tolerate 240-500 ml of milk per day, whilst fermented dairy products such as yoghurt are often better tolerated as the lactose is fermented by the probiotic strains added in the process.[5]
It has been suggested that the symptoms experienced by lactose intolerant patients are the result of a different fermentation of lactose in the colon. When lactose is malabsorbed and enters the colon, it is fermented by the resident microbiota into a variety of metabolites including lactate, formate, succinate and short chain fatty acids (SCFAs) such as acetate, propionate, butyrate, as well as producing gases including hydrogen (H2), carbon dioxide (CO2) and methane (CH4).[7] What is lesser known is that lactose may actually influence the colonic microbiota favourably if it is not digested in the small intestine. Lactose may enhance innate gut immunity not only in early life, but also throughout all life stages via synergistic action with other carbohydrates or SCFAs.[6]
Lactose intolerance leads to symptoms such as bloating, flatulence and diarrhoea as a result of an increased concentration of lactose in the colon. There is evidence proposing that some of the observed symptoms may in fact be an effect of perturbation of the microflora in response to increased expression of cathelicidin antimicrobial peptide (CAMP) in the colon mediated by lactose.[8] This research suggests that lactose may play an integral role in the development of the intestinal microbiota and support the innate immune response of the neonate. The role of antimicrobial peptides, like CAMP are to aid in the defence against invasive bacterial infection. Therefore, we can see that human milk likely possesses a high concentration of lactose in order to protect the neonatal gut against pathogens, whilst also regulating the microbiota of the infant.[8]
ASSESSMENT & DIAGNOSIS
The most common testing method to diagnose lactose intolerance is the lactose hydrogen breath test.[2] In some instances confirmation of lactase activity by a duodenal biopsy may be called for.[5] It is argued however, that humans would never ingest pure lactose, meaning that a ‘lactose tolerance test’ is not what is required for present public health or clinical purposes.[6]
CONCLUSION
Lactose may have been unnecessarily demonised whilst overlooking the very important, and evolutionary reasons for its inclusion in food supply. What seems to be more of an issue is how insidious it has become, particularly in processed foods, and therefore the volumes and frequency with which it is now consumed. More evidence is also warranted to determine whether modern processing techniques play a role in the rise of dairy or lactose intolerance.
KEY PRACTICE POINTS [6]
- Breast-fed infants derive a major portion of their energy intake from lactose and it plays an important role in the maturation of innate immunity.
- Regardless of lactate status, lactose may be consumed in the diet in modest amounts (up to 12-24 g per day) ideally in small amounts across the day.
- Lactose-free or lactase-supplemented foods are not necessary for those in whom lactase activity is not persistent beyond infancy.
- Lactose may favourably alter the colonic microbiota if it is not digested in the small intestine.
- Lactose may enhance innate gut immunity not only in early, but also later life through synergistic action with other carbohydrates or SCFAs (e.g. butyrate)
- Lactose avoidance can be challenging and may unnecessarily restrict nutrient dense foods. It may be more prudent to restrict consumption to levels below 12g per day.
REFERENCES
- Roy Morgan Research. Lactose intolerance on the rise amongst Australian Women. Roy Morgan Research 2016. Viewed 1 April 2016. [Link]
- Lomer M, Parkes G, Sanderson D. Review article: lactose intolerance in clinical practice - myths & realities. Alimen Pharm & Ther 2008; 7(2):93-103. [Full Text]
- Heyman M. Lactose intolerance of infants, children and adolescents. Pediatrics 2006; 118(3):1279-1286. [Full Text]
- Eadala P, Matthews S, Waud J, et al. Association of lactose sensitivity with inflammatory bowel disease - demonstrated by analysis of genetic polymorphism, breath gases and symptoms. Aliment Pharm & Ther 2011; 34(7):735-746. [Full Text]
- Vandenplas, Y. Lactose intolerance. Asia Pac J Clin Nutr 2015;24(1):9-13. [Full Text]
- Lukito, W. Malik, S. Surono I, et al. From ‘lactose intolerence’ to ‘lactose nutrition’. Asia Pac J Clin Nutr 2015;24(1):1-8. [Full Text]
- Windey K, Houben E, Deroover L, et al. Contribution of colonic fermentation and fecal water toxicity to the pathophysiology of lactose-intolerance. Nutrients 2015; 7(9): 7505-7522 [Full Text]
- Cederlund A, Kai-Larsen Y, Printz G, et al. Lactose in human breast milk an inducer of innate immunity with implications for a role in intestinal homeostasis. PLoS One 2013;8(1):e53876 [Full Text]
DISCLAIMER:
The information provided on FX Medicine is for educational and informational purposes only. The information provided on this site is not, nor is it intended to be, a substitute for professional advice or care. Please seek the advice of a qualified health care professional in the event something you have read here raises questions or concerns regarding your health.