Today we are joined by nutritionist Jessica Cox who shares her clinical approach to how, when and why you might incorporate microbiome testing with your patients.
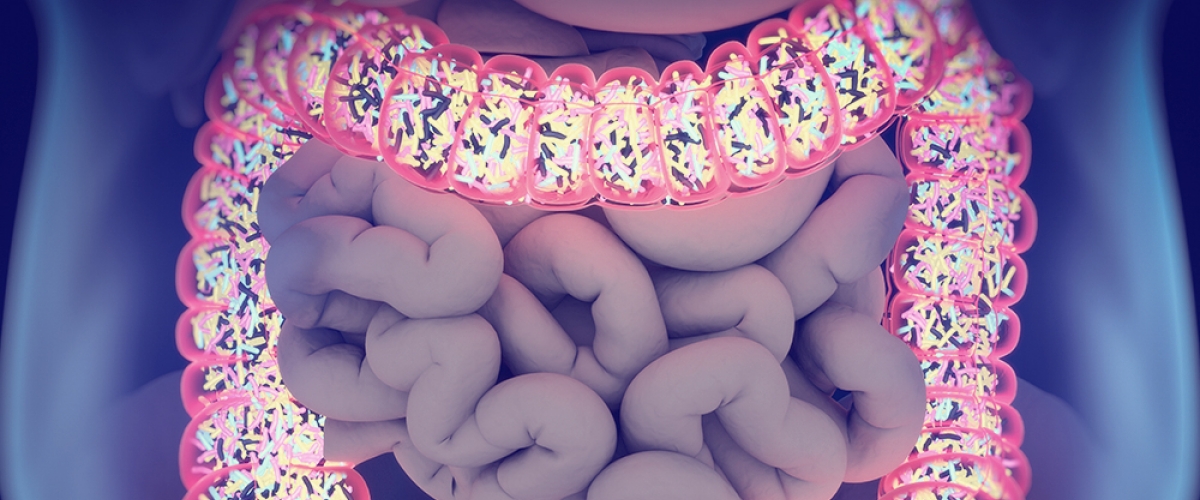
Dr Van Den Bogaerde shares the current scientific opinion on gut microbial diversity and he discusses his excitement about the research exploring faecal microbial transplants
The coconut palm tree, fruit and oil (Cocus nucifera) have a long history of use in Malaysia, India, the South Pacific and the Philippines for many religious, dietary and medicinal purposes.[1,2] The multifaceted application of coconut by traditional paradigms has also been observed in recent years with a resurgence in the popularity of coconut oil, particularly for dietary and medicinal purposes.[1,3,4]
Emerging research indicates that an abnormal gut microbiome is a predisposing factor in the development of neurodevelopmental disorders, including autism spectrum disorder (ASD).[2,3] A growing number of studies have found that children with ASD have a gut microbiome that differs from that found in neurotypical children, indicating a link between gut and brain function.[4-8]
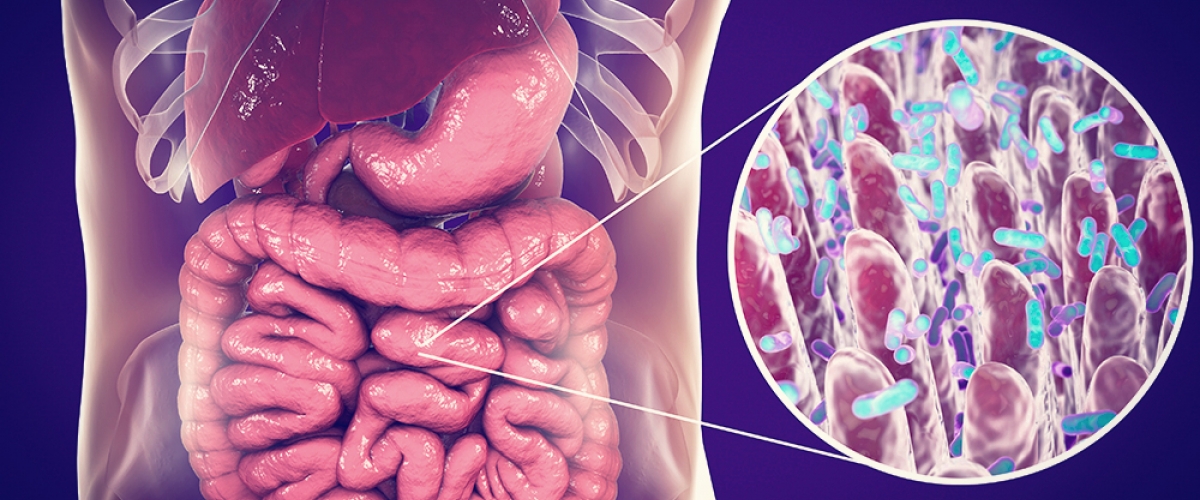
The intestinal microbiome is a complex signalling hub that incorporates environmental factors, such as diet, stress and xenobiotics, with genetics and immune signals to influence host immunity and response to infection.[1-3] Within the last decade, we have begun to understand the importance of this interdependent bilateral interaction between the host and its microbiota and how its mutually beneficial balance is crucial in host defence and immune health.[1]
Could polyphenols and their influence on microbiota be an effective strategy for the prevention of neurodegeneration? Polyphenols are naturally occurring compounds in many berries, fruits and vegetables, as well as cereals, tea, coffee, cocoa, and wine. Polyphenols suppress neuroinflammation and protect neurons against oxidative stress and inflammatory injury, thus promoting memory, learning, and cognitive functions.
Mention quercetin and the first thing that will spring to mind for practitioners will most likely be its efficacy in the treatment of allergies. Often referred to as ‘nature’s antihistamine’, quercetin reduces the allergic response by stabilising mast cells and basophils thus preventing the release of histamine.
The role of Blastocystis hominis (BH) as a pathogen in the human body is shrouded in controversy. Very commonly found in society, this mysterious and elusive parasite still baffles scientific and medical communities. Having an understanding of what is currently known about the BH microbe, and being aware of the use of non-pharmaceutical measures, will guide many therapists towards safe and effective individual protocols, where treatment, regardless of symptom status, can increase overall health and wellbeing.